Building Trust: Bridging Science and Vaccine Hesitancy |
octobre 16, 2024 . 7 Minutes read
Overcoming Vaccine Hesitancy: A Multifaceted Approach for Global Health (Part 2)
Vaccine hesitancy remains a critical challenge to global health. Study research-supported approaches to managing concerns, building trust, and implementing effective strategies to boost vaccine uptake and help maintain public health.
Global Variations in Vaccine Acceptance
Addressing vaccine hesitancy is a multifaceted approach, and healthcare providers 's role in building vaccine confidence, countering misinformation, and promoting evidence-based vaccine recommendations is crucial. [1]
According to a systemic review in 2021, COVID-19 vaccine acceptance rates vary significantly across countries, ranging from 23.6% in Kuwait to 97% in Ecuador. [2] A blog from the World Bank presents that the highest levels of vaccine hesitancy were observed in Eastern European and Central Asian countries, while the lowest was in Latin American and Caribbean countries. [4]
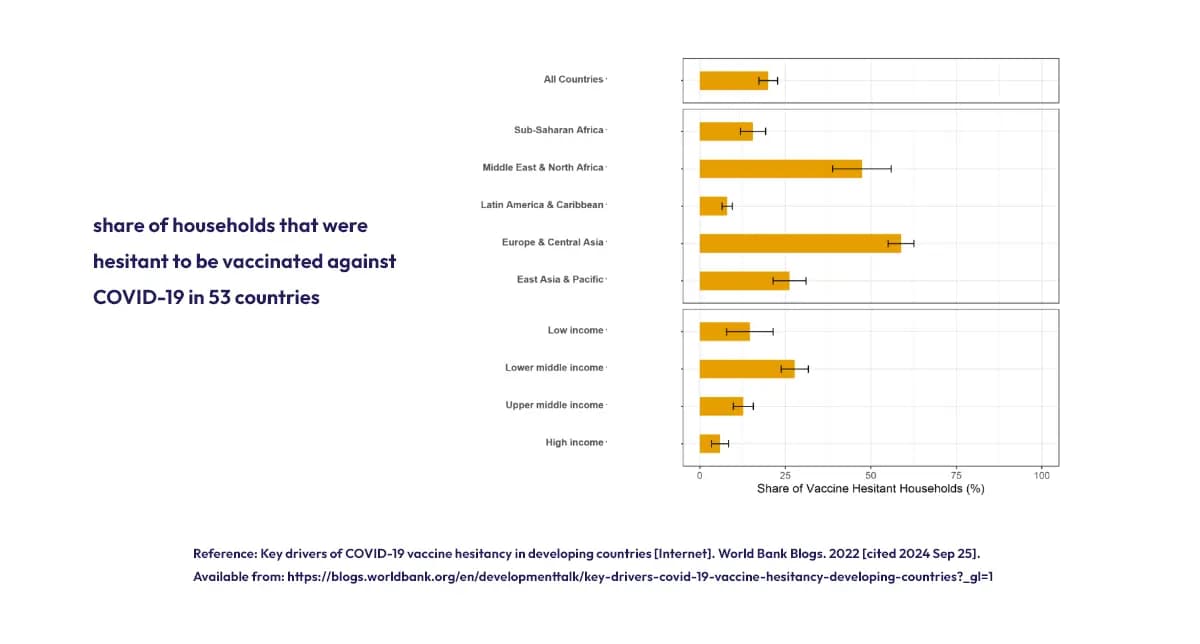
Vaccine hesitancy rates vary across 53 countries, with the highest in Europe and Central Asia and the lowest in Latin America and the Caribbean.
Identifying key sources of vaccine hesitancy is critical to enhancing vaccination rates.
The Critical Role of Addressing Vaccine Hesitancy
Studies show that while social and structural inequities are major factors in vaccination disparities, addressing social and structural barriers to vaccination is not enough to promote population health when psychological factors such as vaccine hesitancy persist. The research report shows that counties with low social and structural barriers but high vaccine hesitancy are projected to have 14% lower vaccination coverage. The findings suggest that identifying key sources of vaccine hesitancy within each county, regardless of its vulnerability, is crucial for developing targeted interventions for future pandemics. [3]
A blog from the World Bank indicates the following main reasons for vaccine hesitancy:
- Concerns over safety, especially worries about side effects
- Mistrusts about vaccine effectiveness
- General dislike of vaccines
- Preference for innate immunity [4]
Strategies for Healthcare Providers to Address Vaccine Hesitancy (Part 1)

Effective provider-patient communication is key to addressing vaccine hesitancy.
Strengthen Provider-Patient Communication:
- Enhance Communication Skills: Participate in communication skills training to engage respectfully and effectively with vaccine-hesitant individuals. Avoid crude and sarcastic language, as it is often counterproductive.
- Encourage Open Dialogue: Create a safe space for patients to express their concerns and ask questions without worry of judgment. Active listening and empathetic responses are critical. [1 & 5] Spend more time with patients during appointments and consider and respect the differences in vaccine hesitancy reasons among different ethnic groups, such as lack of reliable information and cultural/religious factors. [6]
- Address Concerns and Misconceptions: Use clear, non-technical language to provide evidence-based information to clarify common vaccine concerns.
- Develop Culturally Sensitive Materials: Develop educational resources that respect cultural perspectives and preferences to improve understanding and trust. [1 & 5]
- Clarify the safety of Vaccine Components: Explain the safety and purpose of vaccine ingredients, such as aluminum adjuvants. For instance, in his case, you can highlight that while aluminum adjuvants may cause mild local reactions, they pose an extremely low risk to infants, as confirmed by the FDA. [7]
- Discuss Immunity Risks: Compare the risks of acquiring immunity through disease versus the controlled protection provided by vaccines, emphasizing the benefits of vaccination.
- Use Motivational Interviewing: Apply motivational interviewing techniques to explore and address individual vaccine concerns and collect information to gain insights about the perceptions, behaviors, attitudes, and knowledge of the hesitant population. This interview helps foster a more personalized and effective dialogue.
- Leverage Diverse Communication Channels: Use a mix of traditional and digital media to reach different demographic groups, especially those distrusting the healthcare system. Engage through community meetings, social media, and local events. [1 & 5]
Strategies for Healthcare Providers to Address Vaccine Hesitancy (Part 2)
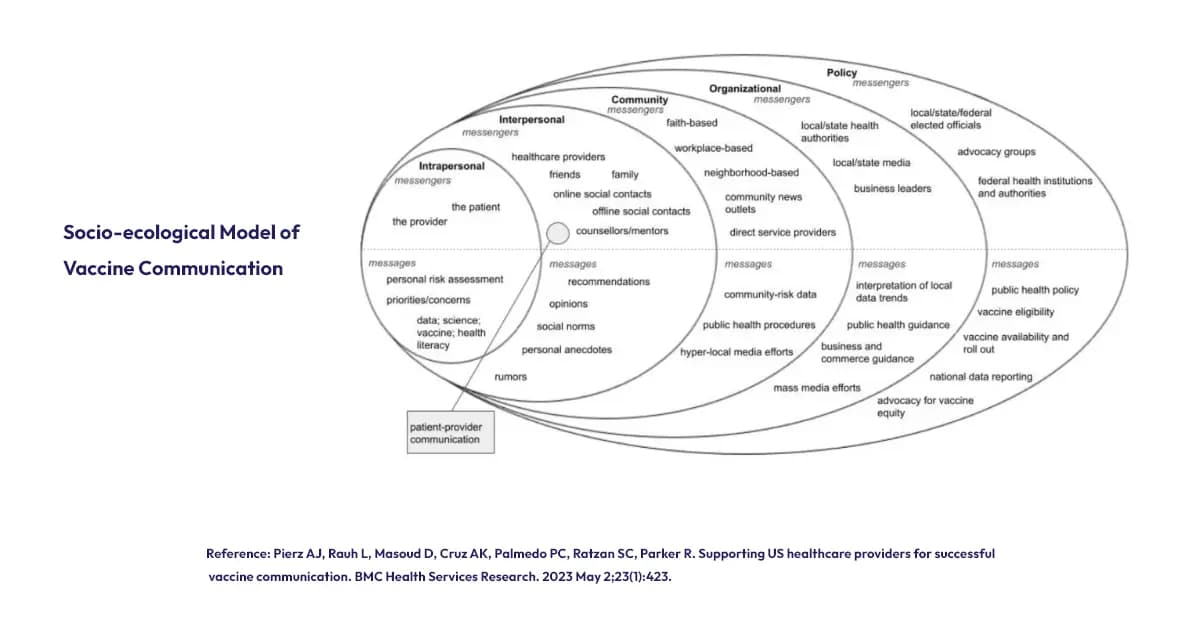
Socio-ecological model for effective vaccine communication across communities.
Engage the Community and Implement Broad-Based Strategies:
- Implement Community-Based Strategies: Involve communities in planning vaccination programs, considering their input on locations, times, and cultural concerns. This collaborative approach can enhance trust and acceptance.
- Utilize Community Influencers: Collaborating with community leaders, spiritual figures, and reputable public personas can significantly promote vaccine trust and address misinformation in culturally relevant ways. [1]
- Leverage Community and Organizational Resources: Collaborate with local health units and professional organizations to stay updated with the latest information and receive regular updates and resources for effective communication with patients and for staying current amidst changing guidelines.
- Advocate for Policy-Level Support: Promote free or low-cost vaccination to reduce financial barriers. Help vaccines be accessible at convenient locations, such as portable units and pharmacies, to remove logistical barriers and increase vaccination uptake. Offer flexible clinic hours, including evenings and weekends. [1 & 5]
Strategies for Healthcare Providers to Address Vaccine Hesitancy (Part 3)

Continuous education for healthcare providers is key to reducing hesitancy and improving vaccine uptake.
Leverage Cost-Saving Behavioral Insights:
- Default appointments: A recent study found that automatically scheduling patients for flu shots (with the option to opt out) increased vaccination rates by 10% at a large medical practice. [8] Additionally, a randomized clinical trial involving 11,188 patients demonstrated that text messaging significantly improved vaccination rates. Notably, messages that gave patients a sense of ownership, such as 'a flu shot has been reserved for you,' were more effective than generic messages like 'flu shots will be available.' [9]
- Social norms messaging: Studies show that providing normative information in vaccine communications and the widespread acceptance of vaccination (such as We estimate that, based on survey responses from last month, X% of individuals in your country indicated they would receive a vaccine if it becomes available) relatively corrects individuals' devaluation of how many others will accept a vaccine. [10]
Strategies for Healthcare Providers to Address Vaccine Hesitancy (Part 4)

Continuous education for healthcare providers is key to reducing hesitancy and improving vaccine uptake.
Continuous Education:
- Healthcare providers play a critical role in overcoming barriers to vaccine acceptance. As such, training, especially focusing on improving vaccine uptake, is vital. Continuous professional development and regular training on effective vaccine communication help address patient concerns and reduce hesitancy. [1]
- Altogether, addressing vaccine hesitancy requires a multifaceted approach combining effective communication strategies, evidence-based practices, and continuous professional development. By implementing these strategies, healthcare providers can play a crucial role in boosting vaccine confidence and improving immunization rates.
Beyond Hesitancy: CIMA Care's Commitment to Global Vaccination
As illustrated, CIMA Care takes a multifaceted approach to addressing vaccine hesitancy. CIMA Care's digital solutions, including the CIMA app and admin panel, enable data-driven care delivery and informed decision-making. Moreover, to empower healthcare professionals and parents, CIMA Care provides evidence-based resources through targeted health messages and the CIMA Health Academy CPD courses. The CIMA Health Academy (recognized on the CPD UK platform as a member of the CPD Certification Service) provides specialized education that develops healthcare providers' knowledge, vaccine advocacy, and management skills. CIMA Care also facilitates informed choices and optimizes vaccine uptake by combining real-time data tracking, personalized reminders, vaccination history, and targeted educational content. CIMA Care's comprehensive system builds trust in vaccination while offering policymakers valuable insights through data visualization tools like heat maps. This synergy of digital innovation, education, and data analytics creates a robust ecosystem that can make measurable progress in improving vaccination rates and protecting children's health across multiple countries. Join CIMA Care in our mission to overcome vaccine hesitancy and advance global health outcomes.
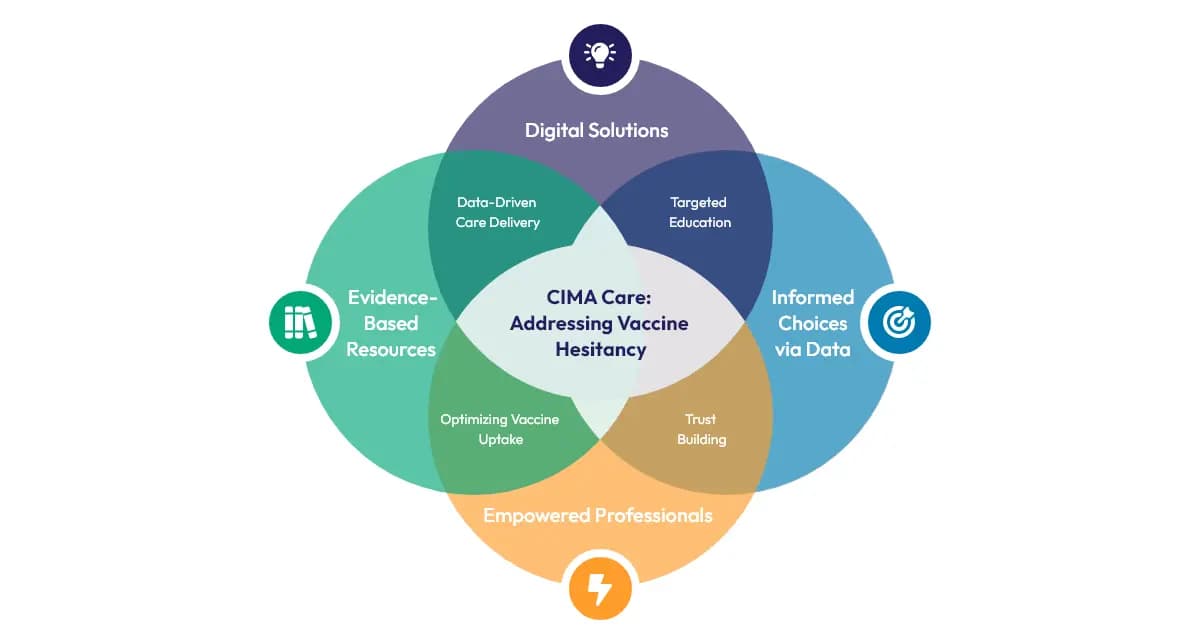
CIMA integrates digital tools, real-time data, and professional growth to address hesitancy and increase uptake.
Image References
- 1- Adobe Stock. Vaccine or no vaccine choice, COVID-19 vaccination concept [Internet]. Adobe Stock; [cited 2025 Aug 18]. Available from: https://stock.adobe.com/fi/images/vaccine-or-no-vaccine-choice-covid-19-vaccination-concept/395999414
- 2- Adobe Stock. A parent holding a young child raises their hand in refusal as a healthcare worker attempts to administer a vaccination in a clinic setting [Internet]. Adobe Stock; [cited 2025 Aug 18]. Available from: https://stock.adobe.com/fi/images/a-parent-holding-a-young-child-raises-their-hand-in-refusal-as-a-healthcare-worker-attempts-to-administer-a-vaccination-in-a-clinic-setting/846771819
- 3- Adobe Stock. African mother and her son in doctor’s office with doctor and nurse [Internet]. Adobe Stock; [cited 2025 Aug 18]. Available from: https://stock.adobe.com/fi/images/african-mother-and-her-son-in-doctor-s-office-with-doctor-and-nu/50872126
-
4- Adobe Stock. Young African American medical workers [Internet]. Adobe Stock; [cited 2025 Aug 18]. Available from: https://stock.adobe.com/fi/images/young-african-american-medical-workers/50868015
Blog Resources
- 1- Goje O, Kapoor A. Meeting the challenge of vaccine hesitancy. Cleveland Clinic journal of medicine. 2024 Sep 4;91(9 suppl 1):S50-6.
- 2- Sallam M. COVID-19 vaccine hesitancy worldwide: a concise systematic review of vaccine acceptance rates. Vaccines. 2021 Feb 16;9(2):160.
- 3- Tolley AJ, Scott VC, Mitsdarffer ML, Scaccia JP. The Moderating Effect of Vaccine Hesitancy on the Relationship between the COVID-19 Vaccine Coverage Index and Vaccine Coverage. Vaccines. 2023 Jul 12;11(7):1231.
- 4- 1.Key drivers of COVID-19 vaccine hesitancy in developing countries [Internet]. World Bank Blogs. 2022. Available from: Key drivers of COVID-19 vaccine hesitancy in developing countries
- 5- Pierz AJ, Rauh L, Masoud D, Cruz AK, Palmedo PC, Ratzan SC, Parker R. Supporting US healthcare providers for successful vaccine communication. BMC Health Services Research. 2023 May 2;23(1):423.
- 6- Savoia E, Masterson E, Olander DR, Anderson E, Mohamed Farah A, Pirrotta L. Determinants of Vaccine Hesitancy among African American and Black Individuals in the United States of America: A Systematic Literature Review. Vaccines. 2024 Mar 7;12(3):277.
- 7- 1.Yandell K. Posts Raise Unfounded Concerns About Aluminum in Vaccines [Internet]. FactCheck.org. 2024. Available from: Posts Raise Unfounded Concerns About Aluminum in Vaccines - FactCheck.org
- 8- Chapman GB, Li M, Leventhal H, Leventhal EA. Default clinic appointments promote influenza vaccination uptake without a displacement effect. Behavioral Science & Policy. 2016 Oct;2(2):41-50.
- 9- Buttenheim A, Milkman KL, Duckworth AL, Gromet DM, Patel M, Chapman G. Effects of ownership text message wording and reminders on receipt of an influenza vaccination: a randomized clinical trial. JAMA network open. 2022 Feb 1;5(2):e2143388-.
- 10- Moehring A, Collis A, Garimella K, Rahimian MA, Aral S, Eckles D. Providing normative information increases intentions to accept a COVID-19 vaccine. Nature Communications. 2023 Jan 9;14(1):126.
Enjoyed this article?
Share it with your friends on LinkedIn: Overcoming Vaccine Hesitancy: A Multifaceted Approach for Global Health (Part 2)
Follow us on LinkedIn for more updates and insights: Cima Care GmbH

