Evidence-Based Analysis: Exploring the Relationship Between Vaccines and Type 1 Diabetes |
mai 20, 2025 . 7 Minutes read
Type 1 Diabetes and Vaccination: Separating Fact from Fiction
As global health initiatives continue to advance our understanding of autoimmune conditions, the relationship between vaccinations and Type 1 Diabetes (T1D) remains an area of significant scientific interest. With increasing T1D incidence rates worldwide and ongoing development of evidence-based prevention strategies, healthcare professionals and families seek clarity on this important topic. T This article examines the robust scientific evidence on vaccination safety in relation to type 1 diabetes, systematically addresses persistent misconceptions through epidemiological data, and explores emerging research into potential protective mechanisms of specific vaccines in diabetes prevention strategies.
Understanding Type 1 Diabetes: Autoimmune Pathology and Global Incidence Patterns
Type 1 diabetes is an autoimmune condition where the immune system mistakenly attacks insulin-producing beta cells in the pancreas, leading to insulin deficiency. This complex disease develops from a combination of genetic susceptibility and environmental triggers, with the exact mechanisms still under investigation.
The global incidence of T1D has been steadily increasing over the past decades, with notable geographic variation reflecting the interplay of genetic and environmental factors (such as viral infections and pesticides) and the urgent need for tailored prevention and management strategies worldwide. Nordic countries, particularly Finland, report the highest incidence rates, exceeding 60 new cases per 100,000 person-years, while rates in Asian and African populations remain substantially lower. [1 & 2 & 3]
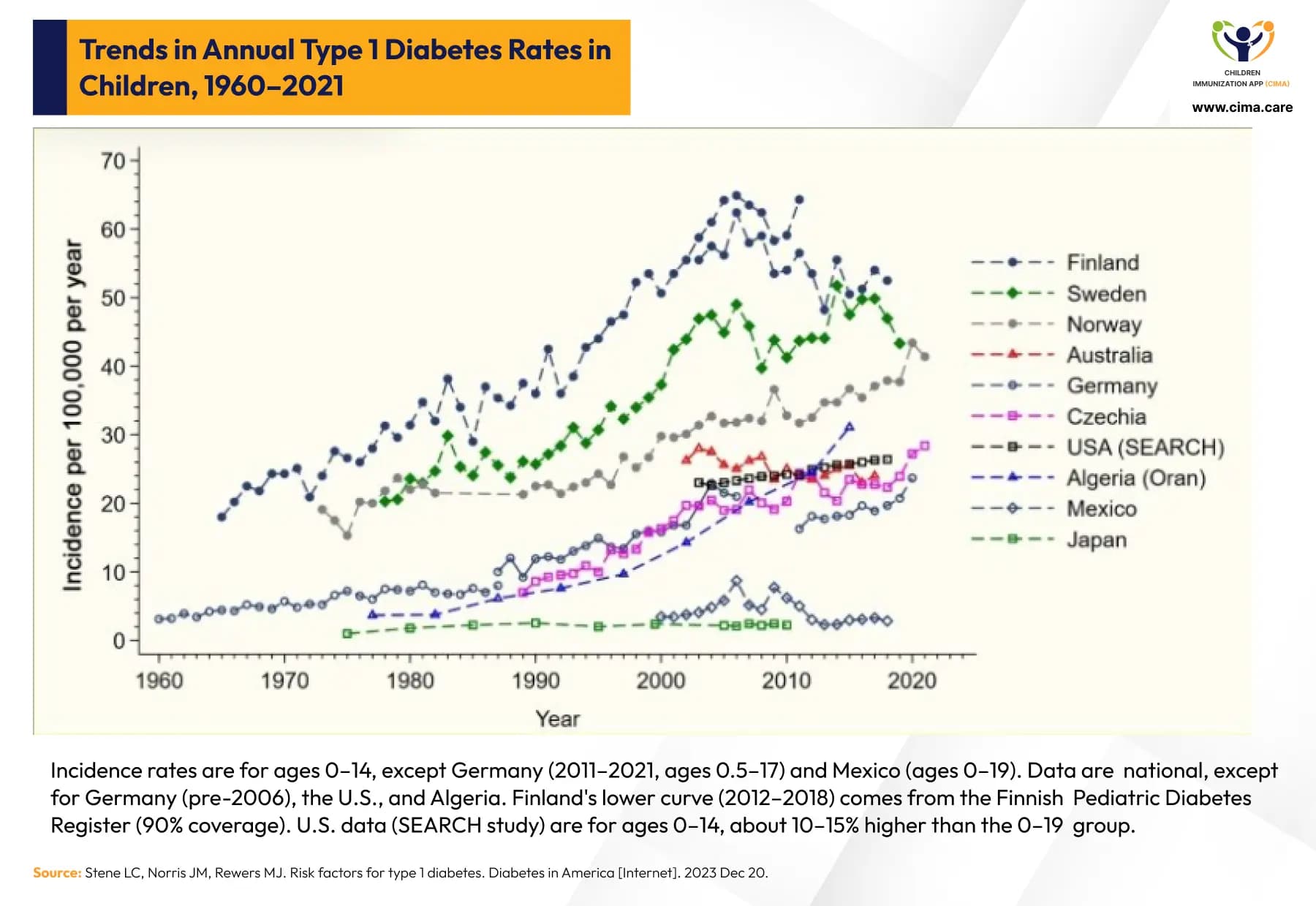
Global T1D incidence trends (1960-2020) showing Finland's peak of 60+ cases per 100,000 person-years.
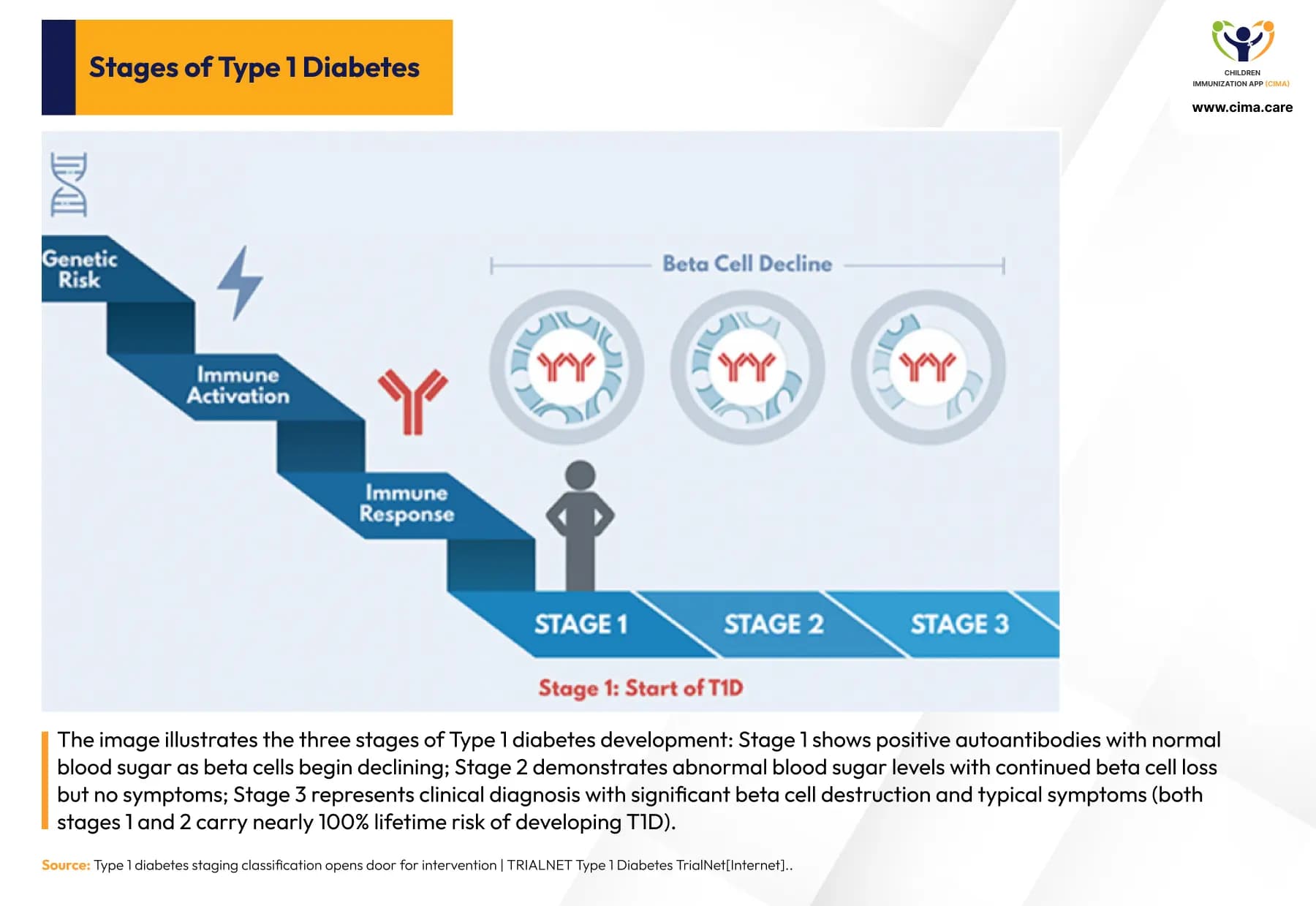
Three-stage progression of type 1 Diabetes: from autoantibody presence to clinical diagnosis.
The Progression of T1D: Understanding Disease Stages
Current scientific evidence indicates that T1D develops in three distinct stages:
- Stage 1: Presence of autoantibodies with normal blood glucose levels.
- Stage 2: Persistent autoimmunity with abnormal glucose metabolism.
- Stage 3: Clinical diagnosis with typical symptoms requiring insulin therapy.
Early detection during Stages 1 or 2 provides an opportunity to prevent diabetic ketoacidosis (a condition where the body burns fat for energy instead of glucose, causing ketone buildup and dangerously acidic blood) and preserve remaining beta-cell function, potentially leading to better long-term health outcomes. [4]
The Scientific Evidence: Childhood Vaccines and T1D
Multiple large-scale epidemiological studies have thoroughly investigated the relationship between childhood vaccinations and T1D risk. The current scientific consensus, based on extensive research, finds no causal relationship between routine childhood immunizations and the development of type 1 diabetes. However, a 2021 review study notes that immune response to vaccines may be less robust in T1D patients due to inherent immune dysregulation, potentially reducing clinical efficacy. For instance, studies report diminished antibody titers post-vaccination (e.g., 58 ± 112.9 mIU/mL in T1D vs. 78 ± 80 mIU/mL in controls for hepatitis B). Despite this, vaccination remains critical for T1D children, who face elevated risks of severe infections. [5]

No link between vaccines and T1D; immunization remains vital for children with diabetes due to higher infection risk.

Scientific evidence is clear: analyzing 739,694+ children across multiple studies confirms vaccines do not cause type 1 diabetes.
Landmark Studies Providing Critical Evidence
The 2004 Danish cohort study by Hviid et al. remains the largest and most methodologically rigorous investigation into childhood vaccinations and type 1 diabetes (T1D) risk. The study of nationwide registry data from 739,694 children found no statistically significant association between routine immunizations (e.g., Hib, MMR, pertussis) and T1D development, with rate ratios consistently close to 1.0 (range: 0.91–1.14). This study's unique strength comes from tracking all Danish children as they received vaccines and monitoring their health outcomes in real time, avoiding the memory errors and researcher bias that often affect smaller studies designed to prove specific theories. [6]
Subsequent research, including systematic reviews and meta-analyses, has reinforced these findings, confirming that vaccines do not increase T1D risk, even in genetically susceptible subgroups. A comprehensive 2021 review published in PubMed Central and the Children's Hospital of Philadelphia Vaccine Education Center's 2024 update both confirm the scientific consensus: multiple studies examining millions of children have found no credible evidence that vaccines cause type 1 diabetes. [7 & 8]
Key Distinctions in Immune Responses
Vaccines safely train the immune system to recognize pathogen components (antigens) without triggering harmful autoimmune reactions, as they use controlled exposure to stimulate protective memory cells and antibodies. [9]
The immune system process differs fundamentally from the dysregulated immune response in type 1 diabetes (T1D), where genetic susceptibility (notably in the human leukocyte antigen [HLA] region) and environmental triggers (e.g., enterovirus infections, rapid early-life weight gain) drive autoimmune destruction of insulin-producing β-cells. Unlike vaccination, T1D involves self-reactive immune cells that mistakenly target pancreatic cells, a process amplified by HLA variants and environmental factors. [10 & 11]

Vaccines train the body's immunity safely without triggering harmful autoimmune reactions, which happen in T1D.
Rotavirus Vaccination: Evidence of Protective Effects Against Type 1 Diabetes
While most research shows vaccines do not increase T1D risk, emerging evidence suggests some vaccines might actually have protective effects. The rotavirus vaccine has received particular attention in this regard.
A 2025 meta-analysis of 4.4 million children across high-income Western countries found that rotavirus vaccination is associated with a 13% reduction in type 1 diabetes (T1D) risk compared to unvaccinated children. [12] This evidence builds on Australian cohort data showing a decline in T1D incidence among children aged 0–4 years after routine rotavirus vaccination began in 2007—the first sustained decrease since the 1980s. Older children (5–14 years) showed no such decline, suggesting the vaccine’s protective effect is specific to early childhood exposures. [13]
Another study in the United States (2001–2017) found a 3.4% annual decline in type 1 diabetes incidence among children aged 0–4 from 2006–2017, aligning with rotavirus vaccine introduction. The findings suggest that rotavirus vaccination may help prevent type 1 diabetes. While causation remains unproven, this aligns with evidence that natural rotavirus infection may accelerate β-cell autoimmunity in genetically predisposed children. Researchers hypothesize that vaccination prevents this trigger by eliminating rotavirus-mediated pancreatic damage or molecular mimicry mechanisms. Molecular mimicry refers to immune cross-reactivity triggered by structural similarities between viral proteins and pancreatic β-cell autoantigens. [14]
Ongoing studies are investigating whether this effect persists into adolescence and applies globally.
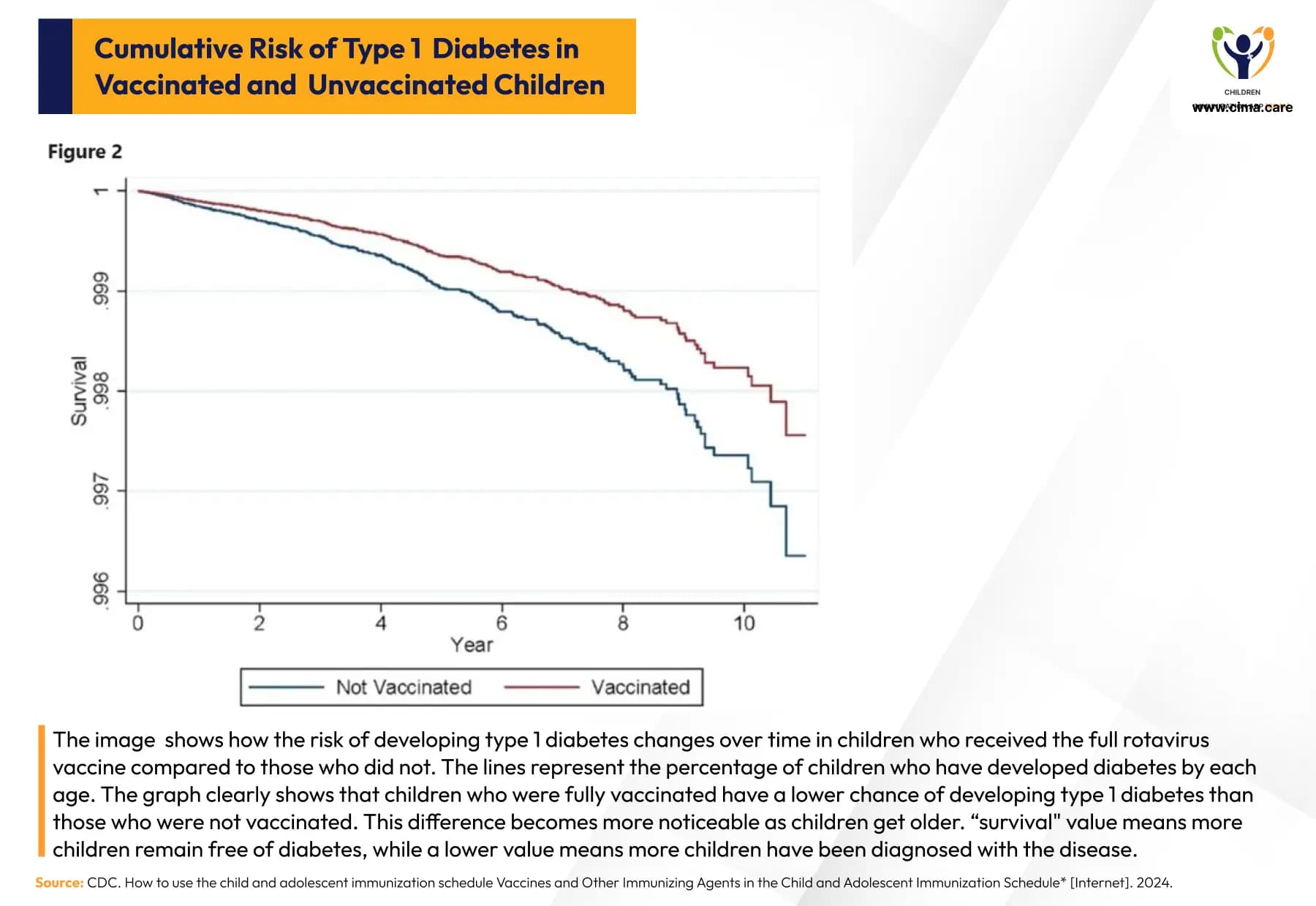
Rotavirus vaccination shows about a 13% reduced T1D risk in children, with sustained protection over time.

Molecular mimicry between rotavirus VP7 and parts of the pancreatic cells GAD65 may trigger autoimmunity in predisposed children.
How Rotavirus Vaccination Works: Preventing Molecular Mimicry and Autoimmune Triggers
Recent research suggests rotavirus vaccination may help protect against Type 1 Diabetes (T1D). Here's why this might happen:
When someone gets infected with natural rotavirus, it can sometimes trigger an autoimmune reaction in children who already have genetic risk factors for T1D. This happens because parts of the rotavirus (specifically a protein called VP7) look similar to parts of pancreatic cells (a protein called GAD65).
This similarity can confuse the immune system, a process called "molecular mimicry." The immune system might first attack the virus, but then mistakenly start attacking the similar-looking pancreatic cells that produce insulin.
By vaccinating against rotavirus, we may prevent this chain reaction from starting in the first place, potentially reducing the risk of developing T1D in vulnerable children.
Current research continues to investigate these protective mechanisms to better understand this relationship. [14 & 15]
BCG Vaccine: New Hope for Treatment and Prevention
The Bacillus Calmette-Guérin (BCG) vaccine, originally developed to prevent tuberculosis, has emerged as a promising therapeutic agent for type 1 diabetes (T1D). Phase III trials (2024) demonstrated that BCG vaccination significantly reduced COVID-19 infections (p < 0.001) and other infectious diseases in T1D patients, with protective effects lasting nearly the entire pandemic period. [16]
BCG vaccine protected T1D patients from COVID-19 and other infections in Phase III trials.
BCG Vaccine: Effects on Blood Sugar and Metabolism
Long-term studies show BCG induces durable metabolic benefits, including a 10% reduction in HbA1c (p = 0.026) sustained for up to 8 years, effectively restoring near-normal blood sugar levels in longstanding T1D patients. The BCG vaccine lowers blood sugar in type 1 diabetes (T1D) by reprogramming immune cells to increase glucose uptake, primarily in the spleen. BCG shifts cellular metabolism from oxidative phosphorylation to aerobic glycolysis—a state where cells rapidly consume glucose. This shift is driven by epigenetic changes (e.g., DNA methylation) in genes regulating glucose pathways, correcting a defect in immune cells’ ability to utilize glucose. The spleen, which showed a 47% increase in glucose uptake over two years, acts as the main site for this metabolic reset, drawing excess glucose from the bloodstream and reducing systemic blood sugar levels. BCG’s persistence in the spleen sustains this effect without restoring insulin production. [17 & 18]
A 2024 analysis of seven studies confirmed that the BCG vaccine can help improve blood sugar control (measured by HbA1c) and reduce certain diabetes-related antibodies in the body, though its effects on insulin production aren't yet clear.[19]
Currently, researchers are conducting advanced trials testing multiple doses of the BCG vaccine, with early results showing better blood sugar management and possible effects on slowing down the diabetes process itself. [20]

The BCG vaccine lowers HbA1c by 10% in T1D patients through immune cell metabolic reprogramming.
Practical Implications for Healthcare Providers and Families(1)
For healthcare providers working with T1D patients, the current evidence offers several important clinical implications:
a. Vaccination Recommendations for T1D Patients
- Children with type 1 diabetes (T1D) should receive all standard immunizations according to their national schedule, as recommended by the CDC and leading diabetes organizations, to reduce their increased risk of infections and related complications. [5]
- Annual influenza vaccination is especially important since children with diabetes are three times more likely to die and six times more likely to be hospitalized due to flu-related complications compared to children without diabetes. [21 & 5]
- On vaccination days, parents and caregivers should be aware that mild fever or the body’s stress response to vaccination can temporarily affect blood glucose levels; therefore, children with T1D may need to monitor their blood glucose more frequently and adjust insulin dosing as needed to maintain glycemic control. [22]

T1D children need all routine vaccines, especially annual flu shots, due to more hospitalization risk.

Healthcare providers must reassure parents that vaccines do not cause T1D and are vital for diabetic children.
Practical Implications for Healthcare Providers and Families (2)
b. Addressing Parental Concerns
Healthcare providers should be prepared to address parental concerns about vaccination and T1D risk with accurate, evidence-based information. Key points to emphasize include:
Multiple large-scale studies have found no link between childhood vaccines and increased T1D risk.
Some vaccines, like the rotavirus vaccine, may potentially offer protection against T1D in certain populations.
Vaccination is especially important for children with T1D, who face higher risks from many vaccine-preventable diseases.
Providing clear, compassionate information builds confidence and encourages vaccination while addressing misconceptions about vaccines and autoimmune conditions like T1D.
Future Research Directions
As our understanding of the complex relationship between vaccines and T1D continues to evolve, several promising research areas are emerging:
- Rotavirus Vaccine Studies: Further research is needed to confirm the potential protective effects of rotavirus vaccination against T1D across diverse populations and to understand the underlying mechanisms.
- BCG Clinical Trials: Ongoing and expanded trials of BCG vaccination for T1D treatment and prevention will help clarify optimal dosing strategies, identify which patients benefit most, and determine the durability of effects.
- Biomarker Development: Identifying reliable biomarkers for vaccine response in T1D patients could help personalize vaccination strategies and monitor protective effects.
- Mechanistic Studies: A deeper investigation into how specific vaccines interact with the immune system in T1D-susceptible individuals will enhance our understanding of both disease pathogenesis and potential intervention points.
- Population Studies: Large-scale, international collaborative studies comparing vaccination programs and T1D incidence across different countries and healthcare systems will provide valuable ecological insights.

Future T1D research: rotavirus/BCG trials, biomarkers, immune mechanisms, global population studies, and more.
Conclusion: Evidence-Based Vaccination Decisions
The scientific evidence clearly indicates that routine childhood vaccinations do not increase the risk of developing T1D. [6 & 8] In fact, some vaccines may offer protection against this autoimmune condition, though more research is needed to fully understand these effects. [12 & 14]
For individuals with established T1D, evidence increasingly supports the safety and importance of recommended vaccinations, [5 & 21 & 22] with potential therapeutic benefits from specific vaccines like BCG. [17 & 19] These findings represent a significant shift in our understanding of vaccine-T1D interactions, moving from concerns about risk to exploration of potential benefits.

Scientific evidence confirms that vaccines don't cause T1D and may even offer protective benefits.
CIMA Health Academy is providing a course on early childhood development, including T1D and a vaccination module.
Looking Forward: Advancing Knowledge and Education
As we continue to advance global health initiatives through evidence-based healthcare practices, the relationship between vaccination and T1D remains an exciting area of research with the potential to improve prevention strategies and treatment options for this challenging condition.
CIMA Health Academy is proud to provide an upcoming comprehensive course on "Child Development During the First 1000 Days of Life," featuring a specialized module on Type 1 Diabetes and Vaccination. This coming course will equip healthcare professionals with the latest research findings and practical strategies for optimizing care during this critical developmental window, integrating the current scientific understanding of vaccination safety and the potential protective effects of vaccination in children with T1D.
Visit www.cima.care to learn more about our ongoing work in digital health innovation, vaccination support, and professional development. Together, we can transform healthcare solutions through knowledge, innovation, and collaboration.
Image References
- 1- Adobe Stock. Doctor using glucometer on patient’s finger [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/doctor-using-glucometer-on-patient-s-finger/118026812
- 2- Adobe Stock. Medical syringe with a needle and a bottle with vaccine [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/medical-syringe-with-a-needle-and-a-bollte-with-vaccine/390008609
- 3- Adobe Stock. Kid receiving COVID vaccine at home [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/kid-receiving-covid-vaccine-at-home/432629051
- 4- Adobe Stock. Crop close-up of male student making notes and studying online [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/crop-close-up-of-male-student-make-notes-handwrite-in-notebook-study-online-on-computer-from-home-man-write-in-notepad-talking-distant-on-webcam-virtual-zoom-call-on-laptop-education-concept/430268143
- 5- Adobe Stock. Shield protect from coronavirus COVID-19 [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/shield-protect-from-coronavirus-covid-19/356211043
- 6- Adobe Stock. Lock on circuit with blinking red lights [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/lock-on-circuit-with-blinking-red-lights/1400409695
- 7- Adobe Stock. Doctor with vial of BCG vaccine for tuberculosis [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/doctor-with-vial-of-the-doses-vaccine-for-bcg-bacillus-calmette-guerin-against-tuberculosis-disease-vaccination-for-booster-shot-for-bcg-bacillus-calmette-guerin-against-tuberculosis-in-the-children/493765943
- 8- Adobe Stock. Close-up diabetic girl with doctor using lancet pen at clinic [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/close-up-diabetic-girl-with-doctor-using-lancet-pen-at-table-in-clinic/1361489324
- 9- Adobe Stock. Nurse making a blood test using glucose meter [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/nurse-making-a-blood-test-man-s-hand-with-red-blood-drop-with-blood-glucose-test-strip-and-glucose-meter/221451341
- 10- Adobe Stock. A glowing lightbulb with arrows symbolizing creative ideas [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/a-glowing-lightbulb-emits-vibrant-arrows-pointing-upwards-symbolizing-bright-ideas-and-creative-solutions-emerging-from-a-central-point-against-a-dark-background/1309316300
- 11- Adobe Stock. Hand placing cube with syringe symbol on vaccination cubes [Internet]. [cited 2025 Aug 17]. Available from: https://stock.adobe.com/nl/images/hand-placing-a-cube-with-a-syringe-symbol-on-top-of-a-line-of-cubes-with-person-symbols-symbolizing-allocation-problem-of-vaccination-on-wooden-background/397944000
Blog Resources
- 1- Mittal R, Camick N, Lemos JR, Hirani K. Gene-environment interaction in the pathophysiology of type 1 diabetes. Frontiers in Endocrinology. 2024 Jan 26;15:1335435.
- 2- New Type 1 Diabetes Statistics Report [Internet]. T1D Strong | Valuable Resources to Help Individuals Thrive with Type 1 Diabetes. 2025. Available from: New Type 1 Diabetes Statistics Report.
- 3- Gong B, Yang W, Xing Y, Lai Y, Shan Z. Global, regional, and national burden of type 1 diabetes in adolescents and young adults. Pediatric Research. 2024 Mar 5:1-9.
- 4- Type 1 diabetes staging classification opens door for intervention | TRIALNET Type 1 Diabetes TrialNet [Internet].www.trialnet.org. Available from: Type 1 diabetes staging classification opens door for intervention | Type 1 Diabetes TrialNet
- 5- Esposito S, Mariotti Zani E, Torelli L, Scavone S, Petraroli M, Patianna V, Predieri B, Iughetti L, Principi N. Childhood vaccinations and type 1 diabetes. Frontiers in Immunology. 2021 Aug 26;12:667889.
- 6- DeStefano F, Mullooly JP, Okoro CA, Chen RT, Marcy SM, Ward JI, Vadheim CM, Black SB, Shinefield HR, Davis RL, Bohlke K. Childhood vaccinations, vaccination timing, and risk of type 1 diabetes mellitus. Pediatrics. 2001 Dec 1;108(6):e112-.
- 7- Glanz JM, Clarke CL, Daley MF, Shoup JA, Hambidge SJ, Williams JT, Groom HC, Kharbanda EO, Klein NP, Jackson LA, Lewin BJ. The childhood vaccination schedule and the lack of association with type 1 diabetes. Pediatrics. 2021 Dec 1;148(6).
- 8- The. Vaccines and Diabetes [Internet]. Welcome | Children's Hospital of Philadelphia. 2019. Available from: Vaccines and Diabetes.
- 9- Pfizer. How Vaccines Work: Immune Response and the Body’s Reaction | Pfizer [Internet]. www.pfizer.com. 2023. Available from: How Vaccines Work: Immune Response and the Body's Reaction | Pfizer
- 10- Noble JA, Erlich HA. Genetics of type 1 diabetes. Cold Spring Harbor perspectives in medicine. 2012 Jan 1;2(1):a007732.
- 11- Quinn LM, Wong FS, Narendran P. Environmental Determinants of type 1 diabetes: from association to proving causality. Front Immunol. 2021; 12: 737964 [Internet]. 2021
- 12- Kosmeri C, Klapas A, Evripidou N, Kantza E, Serbis A, Siomou E, Ladomenou F. Rotavirus Vaccination Protects Against Diabetes Mellitus Type 1 in Children in Developed Countries: A Systematic Review and Meta-Analysis. Vaccines. 2025 Jan 9;13(1):50.
- 13- Harrison PL. Possible link between rotavirus vaccine and decline in type 1 diabetes [Internet]. WEHI. 2019 [cited 2025 May 5]. Available from: Possible link between rotavirus vaccine and decline in type 1 diabetes | WEHI
- 14- Rogers MA, Basu T, Kim C. Lower incidence rate of type 1 diabetes after receipt of the rotavirus vaccine in the United States, 2001-2017. Sci Rep 9 (1): 7727 [Internet]. 2019
- 15- Suliman BA. Potential clinical implications of molecular mimicry‐induced autoimmunity. Immunity, Inflammation and Disease. 2024 Feb;12(2):e1178.
- 16- Century-old Vaccine Protects Type 1 Diabetics from Infectious Diseases [Internet]. Massachusetts General Hospital. 2024. Available from: Century-old Vaccine Protects Type 1 Diabetics from Infectious Diseases.
- 17- Iliyah. Dr Denise Faustman | An Unexpected Ally in the Fight Against Diabetes: The BCG Vaccine • scientia.global [Internet]. scientia.global. 2025. Available from: Dr Denise Faustman | An Unexpected Ally in the Fight Against Diabetes: The BCG Vaccine • scientia.global
- 18- Dias HF, Fu JF, Luck TG, Wolfe GE, Hostetter ER, Ng NC, Zheng H, Kühtreiber WM, Price JC, Catana C, Faustman DL. The spleen assumes a major role in blood glucose regulation in type 1 diabetes patients treated with BCG. Scientific Reports. 2024 Jul 30;14(1):17611.
- 19- Korde SB, Pillewan SR, Dumbre SR, Bandgar AR, Shinde PS, Gairola S, Nikam VS. Significance of Bacillus Calmette-Guerin (BCG) vaccine intervention for patients with Type 1 Diabetes (T1D): A systematic review and meta-analysis. Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 2024 Aug 12:103102.
- 20- New Purpose [Internet]. Harvard University. 2018 [cited 2025 May 5]. Available from: https://hms.harvard.edu/news/new-purpose
- 21- For People With Diabetes, Flu Vaccination is More Important Than Ever - NFID [Internet]. National Foundation for Infectious Diseases - Healthier Lives for All Through Effective Prevention and Treatment. Available from: For People With Diabetes, Flu Vaccination is More Important Than Ever - NFID
- 22- Al-Ozairi E, Irshad M, Taghadom E, Varghese A, Sojan L, Alkandari J. Effect of COVID-19 vaccine on blood glucose metrics in Arabic people with type 1 diabetes. Frontiers in Endocrinology. 2023 Mar 20;14:1120384.
Enjoyed this article?
Share it with your friends on LinkedIn: Type 1 Diabetes and Vaccination: Separating Fact from Fiction
Follow us on LinkedIn for more updates and insights: Cima Care GmbH

